In the riddle about the origin of scar tissue, researchers have reached an important next step. A team led by Helmholtz Zentrum München found that scars are made from a tissue beneath the skin: fascia. This new knowledge led to further discoveries about scarring mechanisms and the fascia matrix which are crucial for the research on scarless skin regeneration and the prevention of fibrosis. The findings were published in Nature journal.
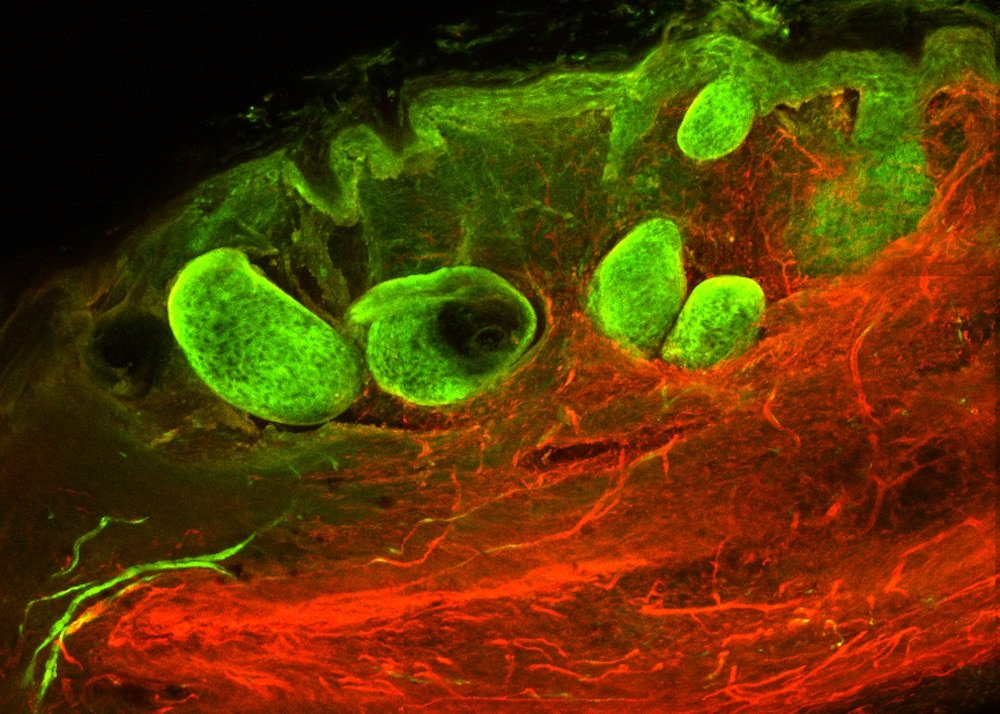
Abnormal scarring is a serious threat resulting in non-healing chronic wounds or fibrosis. Scars form when fibroblasts, a type of cell of connective tissue, reach wounded skin and deposit plugs of extracellular matrix. Until today, the question about the exact anatomical origin of these fibroblasts has not been answered. In order to find potential ways of influencing the scarring process, the team of Dr. Yuval Rinkevich, Group Leader for Regenerative Biology at the Institute of Lung Biology and Disease at Helmholtz Zentrum München, aimed to finally find an answer. As it was already known that all scars derive from a fibroblast lineage expressing the Engrailed-1 gene – a lineage not only present in skin, but also in fascia – the researchers intentionally tried to understand whether or not fascia might be the origin of fibroblasts.
Fibroblasts kit – ready to heal wounds
[ad_336]
In order to find out, they used an array of techniques including genetic lineage tracing, anatomical fate mapping, and genetic ablation, a method which in selected cells leads to apoptosis, cell death. This extinguished the fascia fibroblasts. It was discovered that no matrix was incorporated into the wounds and only abnormal and unhealthy scars with major disadvantages were formed.
In another approach the team placed a porous film beneath the skin to prevent fascia fibroblasts from migrating upwards. This, however, led to chronic open wounds. The researchers concluded that fascia contains a specialized prefabricated kit of sentry fibroblasts, embedded within a movable sealant, that preassemble together all the cell types and matrix components needed to heal wounds. They are assuming that guided homing of fascia initiates the hallmark response to external and internal injuries.
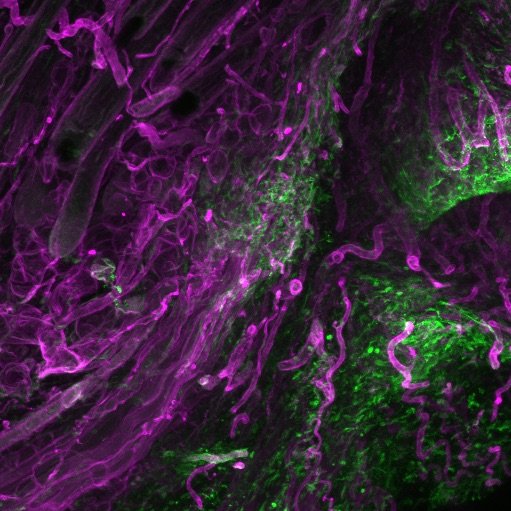
Scarring ensures survival
[rand_post]
The new findings are important in context of ensuring survival: In mammals scarring injury induces a universal fibrotic tissue response that quickly patches wounds with scars – and thus prevents infection and bleeding to death. The hitherto tenet in wound repair was that scars form de novo by fibroblasts depositing extracellular matrix at sites of injury. With this study, the researchers could proof that scars originate from reservoirs of matrix jelly that are dragged into open wounds by sentry fibroblasts embedded in the fascia. These novel findings contradict current paradigms of how wounds repair.
New methods of scarless regenerative healing
The knowledge that fascia is the origin of scars and the finding of new mechanisms of wound repair provide a novel therapeutic space to curtail pathological fibrotic responses and induce scarless regenerative healing across a range of medical settings.
“The findings of our research give fascia tissue a new role for future science. This will shift the attention of the scientific community to not only to look at fibroblasts in the dermis but also at native cells in the fascia when researching on wound healing,” says Rinkevich.
Donovan Correa-Gallegos, PhD student at Helmholtz Zentrum München and first co-author of the study, comments: “Our new findings challenge and reconfigure the traditional view of the body’s matrix system of connective tissue. This is opening up a new biological concept that radiates to a variety of aspects of scar-related disease.”